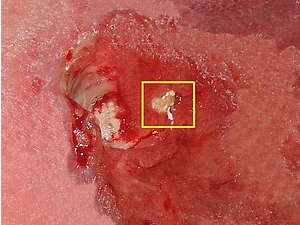
The most popular and topical treatment in the sports world recently is PRP injection therapy. The so-called PRP literally means platelet-rich plasma, that is, plasma with increased concentration of platelets, our first impression of platelets is to help blood clotting, so what does platelets have to do with sports injuries? The reason is that platelets not only help blood to clot, but they are also rich in growth factors that help tissue to grow and repair and heal.
Tissue repair requires blood flow, and blood brings many cells responsible for repair as well as many nutrients, however, tissues like tendons or ligaments do not have a good blood flow supply, so once injured, their ability to repair themselves is poor, and they may grow slowly or not well, therefore, local injections of PRP in damaged tissues will speed up repair, so there are many famous sports stars who have received this treatment after their injuries.
However, not all sports injuries will heal completely after PRP injections, as PRP only provides a beneficial factor to aid in the repair process. As for the final result of the repair, there are still many other factors to consider, such as the degree of damage, the regenerative capacity of the damaged area, the patient’s own physical factors, the patient’s life pattern and nutritional status, the follow-up rehab and sports training, etc. These are all factors that cannot be ignored and are even more important than PRP for the body’s tissue repair.
Therefore, in clinical practice, we often encounter people who have been injected with PRP several times without any progress in their condition. Therefore, patients should have a correct concept that PRP only creates a good repair environment, but the most important thing is to rely on themselves, to follow up the correct rehabilitation and exercise training, and to maintain good living habits and nutritional status, in order to make the best use of the PRP effect.
Rehabilitation Guidelines
- Goal:Protect the injection site and control the pain.
Precautions: You can protect your shoulder with a shoulder strap, protect your wrist or elbow with a parapod, and if the injection site is in the lower extremity, you can walk with crutches with partial weight bearing to reduce the weight on the lower extremity.
Exercise therapy: easy active joint movement is sufficient.
- Goal:Remove immobilization and return to daily activity.
Precautions: slowly remove the immobilized aids or parapods, but do not overextend the tendons and avoid heavy lifting or high-impact activities.
Rehabilitative exercises: Continuous active joint movements, three times a day for five minutes each time; if the upper extremity receives injections, motor training of the lower extremity can be started, if the lower extremity receives injections, motor training of the upper extremity can be started.
- Goal:To achieve full-angle joint movement, strengthen muscle strength and muscle endurance, improve balance and proprioception.
Precautions: Avoid movements that require fast, large angles or high intensity. Large angle or high intensity movements such as throwing, running, jumping, high intensity weight training, strengthening movements, and any movement or activity that causes pain should be avoided.
Rehabilitation exercises: stretch the injured tendon and related muscle groups at least once a day, 3-4 times for each part, 20-30 seconds each time the joint is loosened to a normal functional angle.
Plyometric strengthening exercises, first focus on isometric and centripetal contraction training, slowly increase the intensity to centrifugal contraction training within a tolerable degree, for example: use elastic bands for rotational muscle group training, use dumbbells for wrist and elbow training, single-leg push-ups for knee training, weight lifting for ankle training. The above exercises are recommended to do 3-4 sets of moderate intensity, 6-12 reps per set.
- Goal:Good multi-angle centrifugal and centripetal muscle strength with good dynamic neuromuscular control to achieve the ability to return to the sports field.
Precautions: Soreness after sports training should be relieved within 24 hours.
Rehabilitative exercises: continued plyometric training of the injured area, with a slow increase in resistance, repetitions and frequency.
For upper extremity injuries: Gradually increase the challenge of upper extremity training, including movements that may cause discomfort or instability, and the challenge may include centrifugal contraction, muscular endurance, or speed.
For lower extremity injuries: increase impact control training, starting with single direction training, then adding agility training and gradually increasing agility training.